You’re at risk of developing a diabetic foot ulcer without realizing it. High blood sugar damages your nerves and blood vessels, reducing sensation and slowing healing. Neuropathy affects roughly 90% of ulcer cases, making injuries go unnoticed. Poor blood flow and foot deformities create pressure points for ulcers. Prevention through glucose control, daily checks, and proper footwear matters. Effective treatment combines pressure relief, debridement, and wound care—and understanding your ulcer type shapes your path.
Key Takeaways
- High blood sugar damages nerves and blood vessels, reducing sensation and blood flow, making ulcers more likely to develop.
- Neuropathy weakens foot sensation, so ulcers often develop painlessly and go unnoticed until complications become severe.
- Neuropathic, ischemic, and neuroischemic ulcers each develop from different causes and require tailored treatment strategies for effectiveness.
- Treatment combines pressure off-loading, debridement, antibiotic therapy for infections, and improved glucose control to promote healing.
- Daily foot inspections, proper footwear, regular toenail care, and excellent glycemic control significantly reduce ulcer complications.
What Are Diabetic Foot Ulcers?
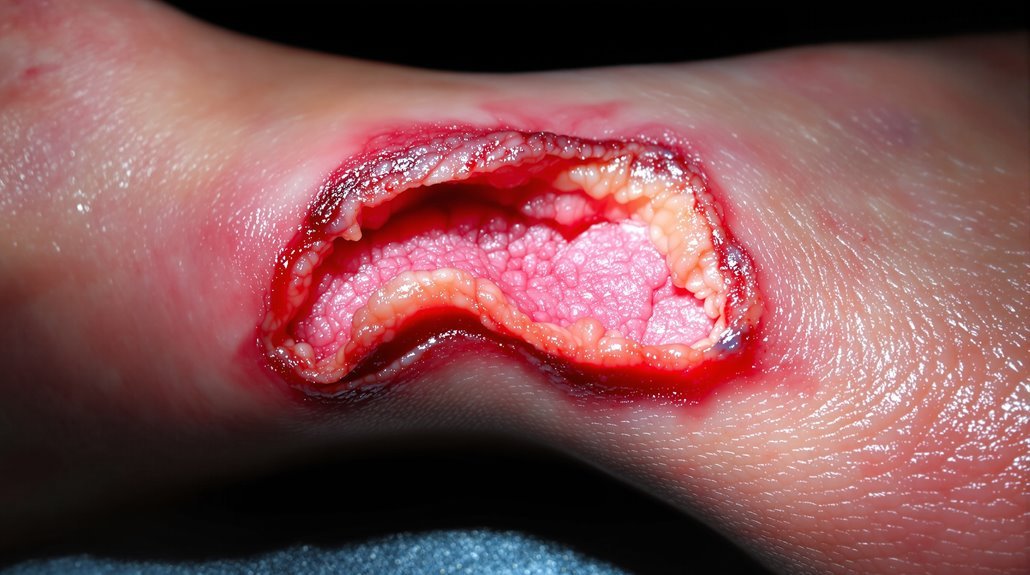
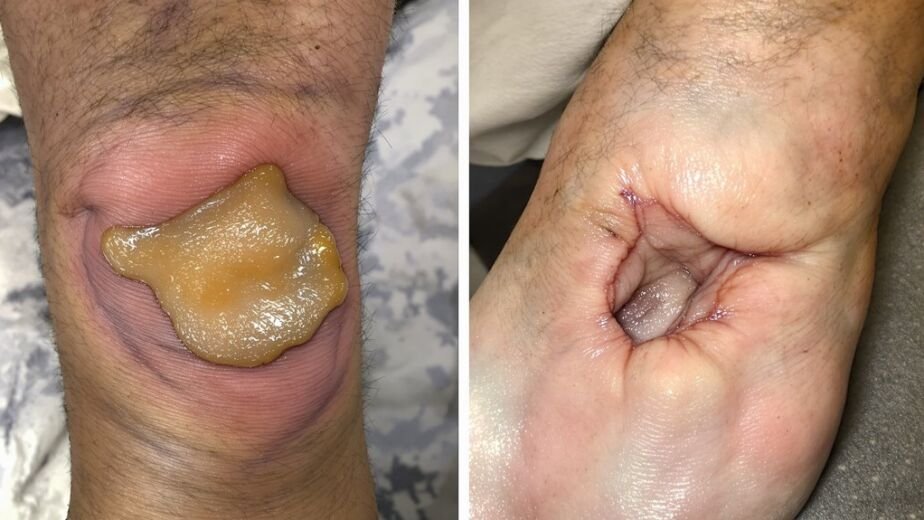
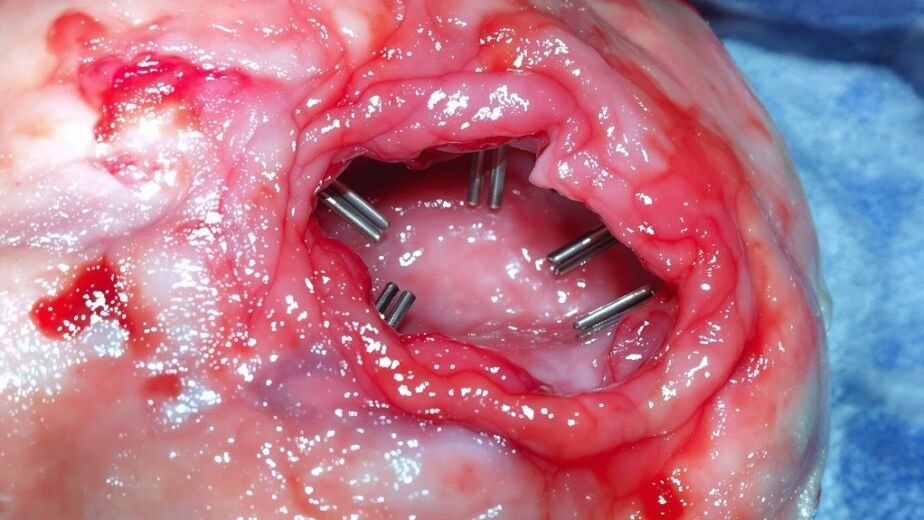
Diabetic foot ulcers are open wounds that form on the feet of people with diabetes, and they’re far more serious than they might initially appear. These painful sores develop when high blood sugar damages nerves and blood vessels—a condition affecting approximately 15% of people with diabetes.
Neuropathy weakens sensation in your feet, so you mightn’t notice injuries until they become severe. Poor blood flow prevents proper healing, creating an environment where infection thrives.
Your symptoms may include swelling, burning pain, and darkened tissue signaling compromised circulation. Early wound care and proper off-loading are critical prevention measures.
Without treatment, diabetic foot ulcers lead to serious complications requiring hospitalization and amputation. Understanding risk factors empowers you to recognize warning signs and seek appropriate care.
Primary Causes of Ulceration
When multiple factors combine, they create the conditions for foot ulcers to develop. Peripheral neuropathy—affecting 90% of ulcer cases—reduces your sensation, so you won’t notice small injuries.
Meanwhile, high blood sugar levels damage your nerves and blood vessels, impairing your healing process. Peripheral artery disease restricts your blood flow, making infection more likely and recovery slower.
You’re also at risk if you have foot deformities or experience trauma. These create pressure points where ulceration begins.
Additional risk factors include poor diabetes management and high plantar pressures. About 15% of people with diabetes experience foot ulcers, but you can change this outcome.
Types of Diabetic Ulcers
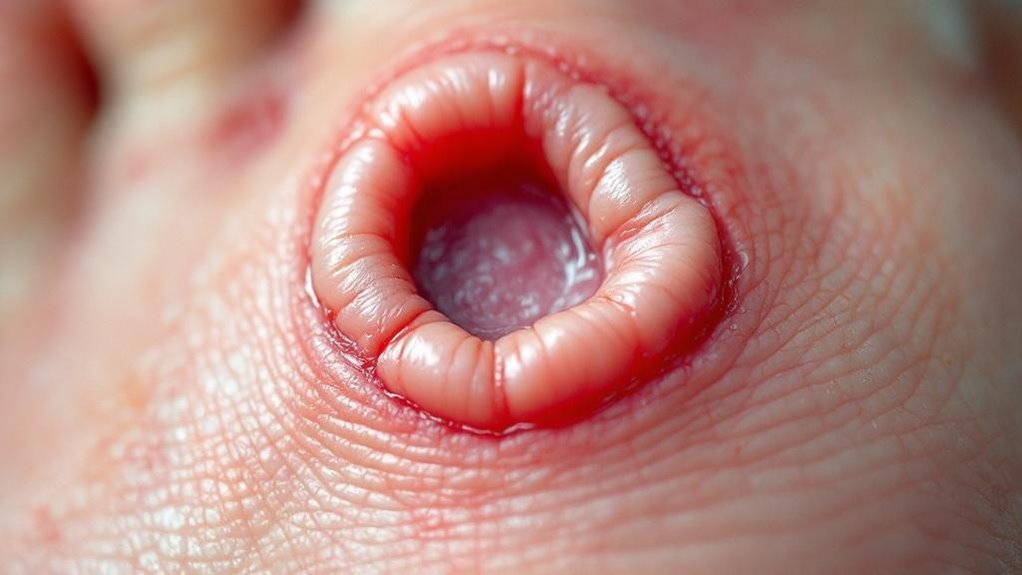
Understanding which type of diabetic foot ulcer you’re dealing with is essential, since each develops through different mechanisms and requires distinct treatment approaches.
Neuropathic ulcers result from peripheral diabetic neuropathy, causing painless wounds you might miss on your plantar surface.
Ischemic ulcers stem from peripheral artery disease, developing in poorly perfused areas on your toes and foot margins.
Neuroischemic ulcers combine both conditions, presenting serious complications.
Proper diagnosis separates these types so you can implement appropriate treatment planning strategies.
Neuropathic ulcers need pressure relief and protection.
Ischemic ulcers require vascular intervention to restore blood flow and prevent tissue damage.
Neuroischemic ulcers demand thorough management addressing both problems simultaneously.
Recognizing these distinctions helps you prevent serious complications like gangrene and determine effective patient recovery paths.
Risk Factors and Who Is Most Vulnerable
Your risk of developing a diabetic foot ulcer depends on multiple interconnected factors that extend well beyond your diabetes diagnosis alone.
Diabetic neuropathy, which affects nearly 90% of all ulcer cases, strips away your protective sensation—key symptoms go unnoticed until injuries worsen considerably.
Peripheral artery disease restricts blood flow to your feet, making healing slower and complications far more severe.
Poor glycemic control accelerates these complications, while a personal history of foot ulcers marks you as especially vulnerable.
Lifestyle choices like smoking dramatically increase your risk, as do advancing age and insulin dependence.
Certain populations—including Native Americans, African Americans, and Hispanics—face disproportionate vulnerability.
Understanding these interconnected risk factors helps you recognize when you need professional treatment and how to protect yourself.
Recognizing Signs and Symptoms
Because diabetic neuropathy often strips away your protective sensation, you can’t rely on pain to alert you to developing problems—making it essential to recognize warning signs yourself before minor irritations progress to serious foot ulcers.
Watch for swelling, redness, and drainage around your diabetic foot, as these are critical signs of infection requiring prompt action. Any visible open sores demand immediate attention, even if they don’t hurt at all.
Check carefully for discoloration, unusual odors, and black tissue indicating poor blood circulation. Regular foot examinations help catch these symptoms early, improving your healing foot’s chances considerably.
The Wagner Ulcer Classification System grades severity from 0 to 5, guiding treatment decisions. By spotting warning signs promptly, you’re protecting someone’s mobility and quality of life.
Treatment and Management Approaches
While diabetic foot ulcers can develop quickly, the good news is that you don’t have to face them without a clear action plan. You’ll want to start by enhancing your glucose control—this foundation supports your body’s natural healing process. Off-loading techniques like specialized footwear and braces relieve pressure on ulcerated areas, allowing your diabetic foot ulcers to heal effectively. Debridement removes dead tissue and debris that prevents ideal healing. You’ll need consistent monitoring and care paired with appropriate wound dressings maintaining a moist healing environment. Regular foot care reduces the risk of serious complications. For severe infections or non-healing wounds, surgical intervention may become necessary. Collaborate with your healthcare team to develop a personalized treatment plan for your unique needs.
| Treatment Approach | Purpose | Benefit |
|---|---|---|
| Off-Loading Techniques | Reduce pressure on ulcer | Accelerates healing |
| Debridement | Remove dead tissue | Promotes tissue regeneration |
| Wound Dressings | Maintain moist environment | Supports healing process |
| Glucose Control | Address metabolic factor | Enhances natural recovery |
| Surgical Intervention | Remove infected tissue | Prevents severe complications |
Prevention and Daily Foot Care
The foundation of preventing diabetic foot ulcers lies in consistent daily foot care. You’ll reduce your risk by conducting daily foot checks, examining between toes carefully.
Make proper toenail care a priority—trim straight across to prevent ingrown nails and infections. Wash your feet daily with warm water, then dry thoroughly. Moisturizing your skin helps maintain integrity, but avoid applying moisturizer between toes.
Trim nails straight, wash daily with warm water, dry thoroughly, and moisturize—avoiding the area between toes.
You’ll need well-fitting shoes and consider therapeutic footwear designed for diabetes management. These reduce pressure points contributing to foot problems.
Regular foot exams with your healthcare provider guarantee early detection.
Don’t walk barefoot, in socks alone, or thin-soled slippers. You’re protecting your feet from injury.
Ulcer prevention starts with these foundational practices that prevent foot complications and demonstrate care for others.
Conclusion
You can prevent serious complications by taking action today. Control your blood sugar carefully—high glucose slows healing and increases infection risk. Check your feet daily for wounds, numbness, or skin changes you’ve missed. Wear supportive shoes, keep your feet clean and dry, and contact your doctor immediately if you notice ulcers forming. You’re not alone in this—with consistent daily care and professional support, you’ll greatly reduce your risk and protect your mobility.