You’ll find specialists assess chronic wounds across multiple systematic parameters. They measure precise dimensions—length, width, and depth—using standardized tools rather than visual estimation, since measurement errors can exceed 40%. They evaluate tissue type, infection signs, exudate characteristics, and surrounding skin condition carefully. Pain assessment and underlying health factors inform treatment decisions. Documentation of these quantifiable data establishes baselines for tracking healing progress. Each parameter layer reveals deeper complexity inherent in specialist clinical decision-making.
Key Takeaways
- Wound dimensions and measurements using standardized tools to track healing progress and identify deterioration over time.
- Tissue type assessment, distinguishing between healthy granulation tissue (red/pink), slough (yellow), and necrotic tissue (black/brown).
- Exudate evaluation including color, consistency, odor, and volume to assess inflammatory state and microbial burden.
- Infection signs detection through increased pain, purulent discharge, redness, swelling, warmth, and foul odor assessment.
- Wound edges and periwound skin evaluation for attachment status, maceration, erythema, and induration indicating complications.
Wound Dimensions and Measurements
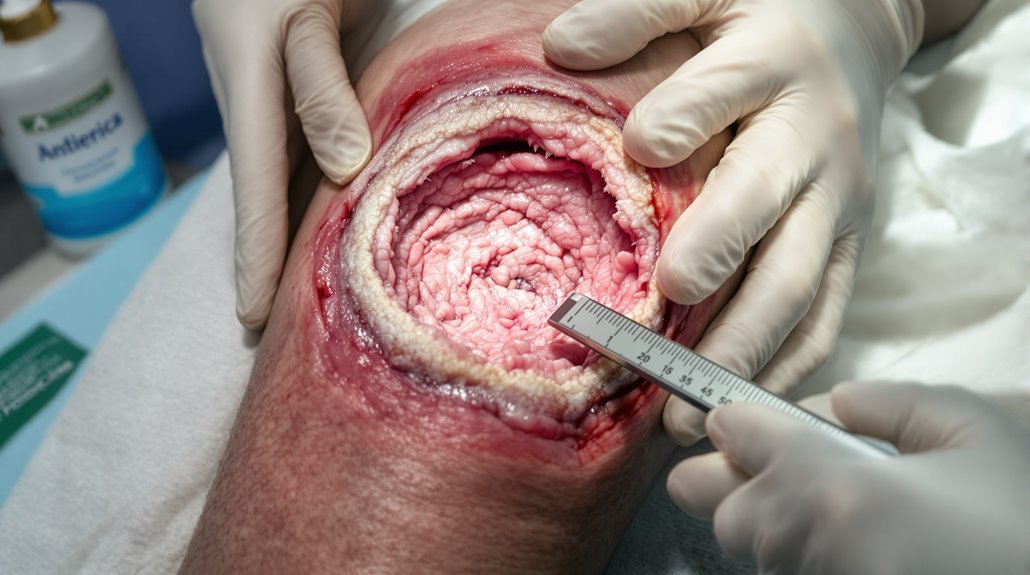
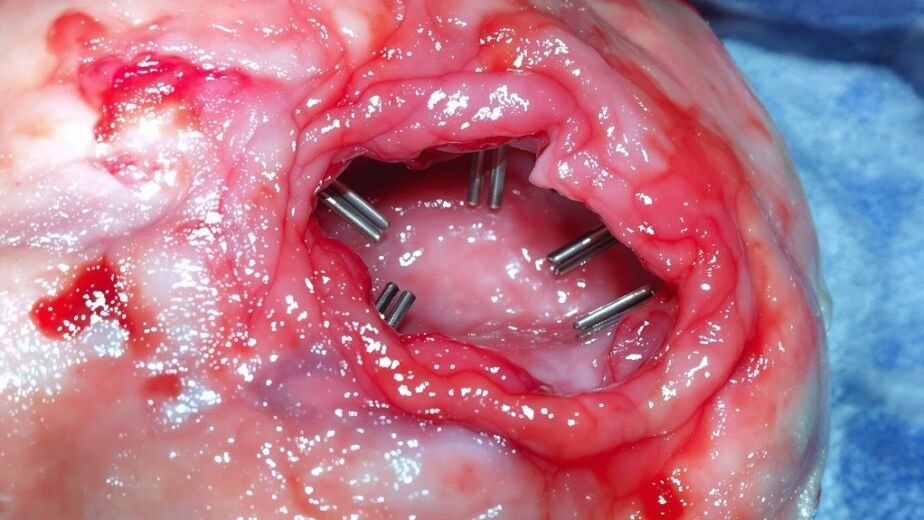
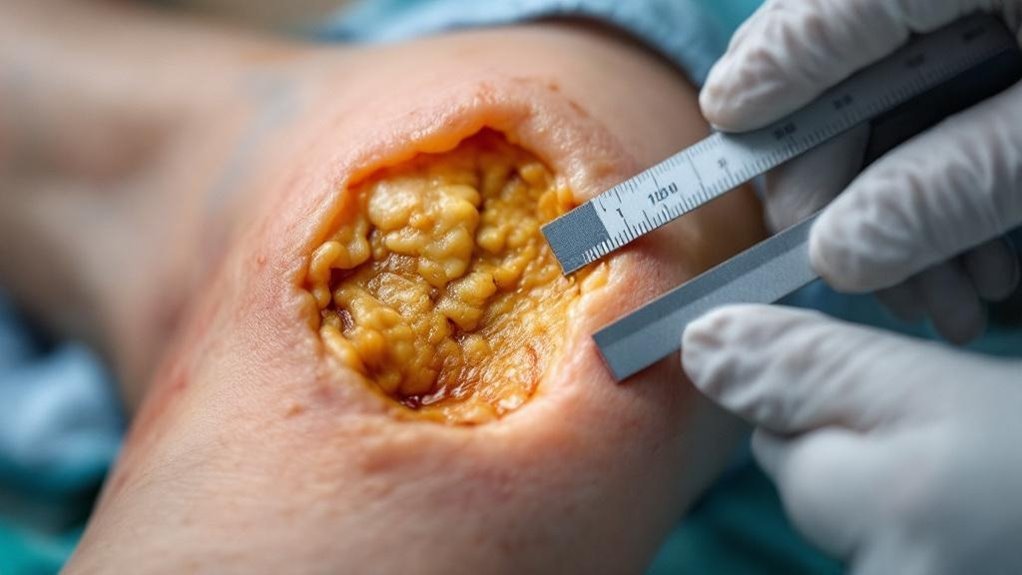
Three dimensions define wound assessment: length, width, and depth. You’ll measure these wound dimensions at each visit using standardized tools like rulers or digital planimetry to guarantee consistency and accuracy.
You’re tracking changes in wound size over time—a reduction indicates positive healing progress and treatment effectiveness. The healing rate directly correlates with dimensional changes; you’ll document these measurements in your wound assessment to guide management strategies.
You’re tracking dimensional changes over time. Wound size reduction indicates treatment effectiveness and guides your management decisions.
You shouldn’t rely on visual estimation alone; studies show measurement errors can exceed 40%. You’re establishing a baseline, then comparing subsequent measurements to evaluate whether your interventions are working.
You’ll record these wound measurements consistently, enabling you to identify deterioration early and adjust treatment protocols. This precision in capturing wound dimensions is essential for optimizing patient outcomes.
Tissue Type and Wound Bed Characteristics
While wound dimensions provide critical baseline data, tissue type and wound bed characteristics offer deeper insight into healing status and treatment response.
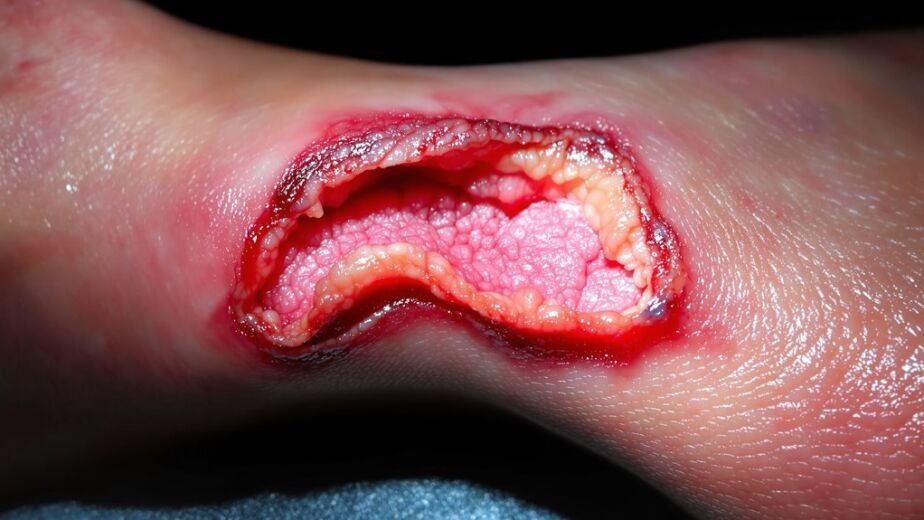
You’ll observe granulating tissue with its beefy red appearance as a positive healing indicator, contrasting sharply with necrotic tissue that appears dark and devitalized.
Evaluate your moisture balance carefully—inadequate moisture signals poor perfusion, while excessive exudate may indicate infection or inflammation requiring intervention.
Assess the wound edge for well-defined, advancing borders that suggest progression, versus irregular or undermined edges indicating complications.
Don’t overlook biofilm presence, which compromises approximately 80% of wound infections and severely impedes healing.
Signs of Infection and Inflammatory Response
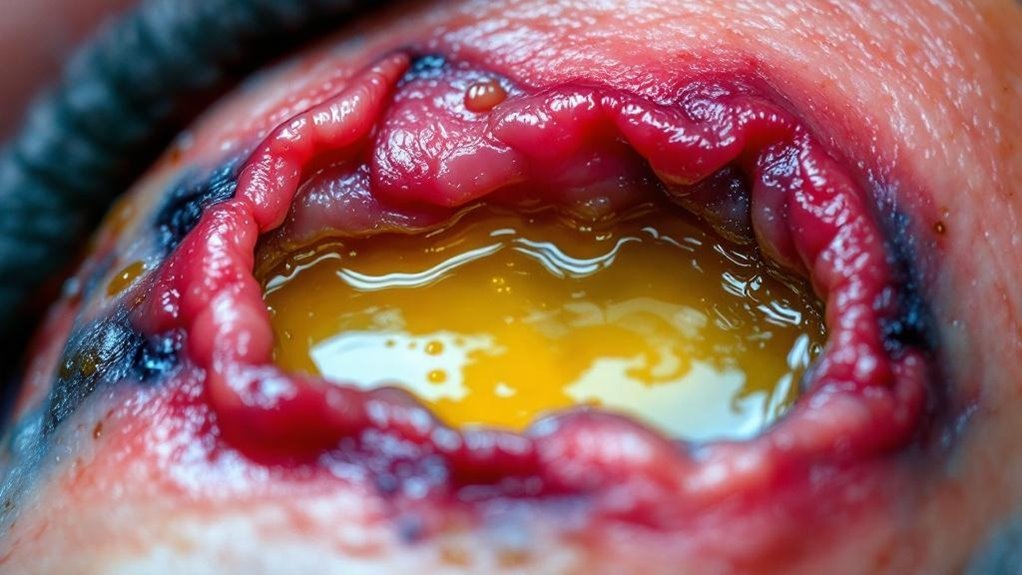
Because distinguishing between normal inflammatory processes and active bacterial infection is critical in chronic wound management, you must learn to recognize the key clinical indicators. Elevated pain levels—especially when progressively worsening—signal inflammatory response and potential wound infections requiring immediate assessment.
You’ll observe increased redness, swelling, warmth, and tenderness surrounding the wound bed. Purulent discharge or strong foul odor indicates bacterial infection demanding prompt intervention.
As a healthcare provider, effective pain management and thorough infection monitoring are your responsibilities, including tracking systemic signs like fever and chills suggesting spreading infection.
Regular assessment of these signs of infection guides your treatment plan adjustments. By tracking inflammatory markers and wound healing progression, you’ll identify when therapeutic modifications become necessary to support recovery in chronic wounds.
Exudate Assessment and Moisture Balance
Exudate assessment extends your infection evaluation, as the characteristics of wound drainage directly reflect the inflammatory state and microbial burden within the wound bed.
You’ll monitor the color, consistency, odor, and volume of exudate to guide your moisture balance strategy. Maintaining this balance is critical in chronic wound care—a moist environment supports epithelial migration and tissue regeneration, while excessive moisture causes maceration and compromises healing.
Overly dry wounds impede healing. You’re seeking a moist wound bed with dry periwound skin for ideal wound outcomes.
When you document exudate changes, you’re identifying shifts in the inflammatory response demanding treatment adjustments. This meticulous assessment helps prevent tissue damage and guarantees your intervention strategy remains aligned with the chronic wound’s needs, serving your patients’ healing goals.
Wound Location and Etiology Classification
Wound location and etiology form a foundational layer of assessment, building on your evaluation of exudate to reveal why a chronic wound developed and how you should direct your treatment strategy.
Understanding the underlying cause notably impacts your wound assessment decisions.
Understanding the underlying cause of a wound fundamentally guides your assessment and treatment strategy.
The four primary etiologies you’ll encounter are diabetic foot ulcers, venous ulcers, arterial ulcers, and pressure ulcers.
Diabetic foot ulcers typically develop on weight-bearing areas with neuropathy, requiring careful monitoring for infection.
Venous ulcers, accounting for 70-90% of chronic wounds, appear on lower legs from venous hypertension.
Arterial ulcers present on distal extremities with exposed tendon or bone, necessitating vascular assessment.
Pressure ulcers develop over bony prominences from sustained pressure.
Each etiology demands distinct interventions and affects tissue damage severity and healing time.
Vascular and Circulatory Status
Since poor circulation impedes the entire healing trajectory, vascular and circulatory evaluation is critical for directing your treatment strategy.
You’ll need to examine blood flow adequacy using diagnostic tools like the Ankle-Brachial Index (ABI) to identify any arterial insufficiency that could considerably compromise your patient’s overall healing potential and long-term outcomes.
This extensive vascular assessment becomes especially important for chronic wound patients, as accurate evaluation determines whether compression therapy‘s appropriate or contraindicated—particularly for arterial ulcers located on distal extremities.
Regular monitoring of your patient’s circulatory health helps you detect venous hypertension early, preventing the development of chronic venous ulcers, the most prevalent wound type.
Surrounding Skin and Tissue Condition
While you’re evaluating tissue perfusion through vascular assessment, you must simultaneously examine the surrounding skin and tissue for multiple indicators of healing compromise.
You’ll assess for signs of infection—redness, warmth, and swelling—that suggest inflammation. Look for maceration, where excessive moisture creates white, waterlogged tissue that compromises barrier integrity.
Inspect for necrotic tissue or slough in adjacent areas; their presence demands debridement to prevent complications. Healthy surrounding tissue should display normal color and texture, indicating adequate blood supply and perfusion.
You’ll also evaluate biofilm formation risks, as up to 80% of wound infections involve biofilm, considerably complicating the healing process.
Any compromised skin near the wound requires preventive measures, as it’s at heightened risk for breakdown. Your thorough examination directly impacts treatment success.
Pain Evaluation and Patient Symptoms
Pain assessment plays a critical role in evaluating chronic wound healing, as increased pain often signals underlying complications such as infection or inadequate tissue repair. You should conduct regular pain evaluation before, during, and after dressing changes to guide your treatment decisions and optimize patient outcomes.
Recognizing signs of infection—including increased pain, redness, swelling, and discharge—prompts immediate intervention. Your patient symptoms assessment directly informs healing progress monitoring and enables you to adjust wound care regimens accordingly.
Implement evidence-based pain management strategies, including appropriate analgesics and topical medications, to enhance patient engagement and compliance. Document pain levels systematically using standardized tools to measure treatment effectiveness.
| Assessment | Key Indicators |
|---|---|
| Pain Quantity | Intensity scale ratings |
| Pain Quality | Character and location |
| Infection Signs | Increased pain, discharge |
Factors Affecting Wound Healing
Chronic wound healing’s success hinges on your ability to identify and manage multiple factors that either facilitate or impede tissue repair.
You’ll encounter intrinsic factors like diabetes and vascular disease that compromise healing capacity, and extrinsic factors including infection, moisture imbalance, and pressure that directly damage tissue.
Biofilm presence complicates approximately 80% of chronic wound infections, requiring aggressive infection control strategies.
Your assessment must evaluate underlying health conditions impairing fibroblast function.
Simultaneously, you’ll address nutritional support through adequate hydration and increased protein intake—essential for ideal wound healing.
Regular pain evaluation guides your proper wound care decisions, as elevated pain signals inadequate tissue repair.
Documentation and Healing Progress Tracking
Systematic documentation of wound characteristics—location, size, depth, and tissue type—establishes your baseline for tracking healing progress and identifying potential complications.
You’ll measure wound dimensions regularly using standardized tools, recording length, width, and depth at each assessment. This quantitative data reveals whether you’re achieving treatment effectiveness and guides adjustments to your care plan.
You’ll document detailed notes on exudate, tissue appearance, pain levels, and signs of infection. Clinical photography captures visual progression, supporting your thorough documentation and enabling clearer communication with your care team.
Conclusion
You’ll systematically evaluate wound dimensions, tissue characteristics, infection signs, exudate levels, and surrounding skin condition during thorough clinical examination. You must classify the wound by etiology—whether it’s arterial, diabetic, pressure, or venous—based on location and appearance. You’re examining tissue type, evaluating pain, and identifying healing impediments carefully. You’ll track surface area reduction: if you don’t achieve 50% reduction within 4 weeks of standard care, you’ll need to reassess and modify your treatment strategy.