You’ll benefit from debridement because it removes dead, damaged, or infected tissue blocking wound healing. Whether you’re dealing with chronic wounds, pressure sores, or burns, debridement accelerates recovery and prevents serious infections. Various methods exist—from surgical techniques using sterile instruments to autolytic approaches using moisture dressings. Each suits different wound types. The procedure stimulates wound edges and creates conditions for tissue regeneration. Learning more about these techniques will help you choose the best option.
Key Takeaways
- Debridement is the removal of dead, damaged, or infected tissue using various specialized techniques to promote healing.
- Debridement is critical for preventing serious infections and promoting wound healing in both acute and chronic wounds.
- Multiple debridement methods exist—surgical, enzymatic, autolytic, biological, and mechanical—each suited for different wound types and conditions.
- Surgical debridement rapidly removes infected tissue under anesthesia, while autolytic debridement uses the body’s natural healing processes.
- Proper aftercare including wound cleaning, moist dressings, adequate nutrition, and follow-up appointments ensures optimal healing outcomes.
Understanding the Debridement Process
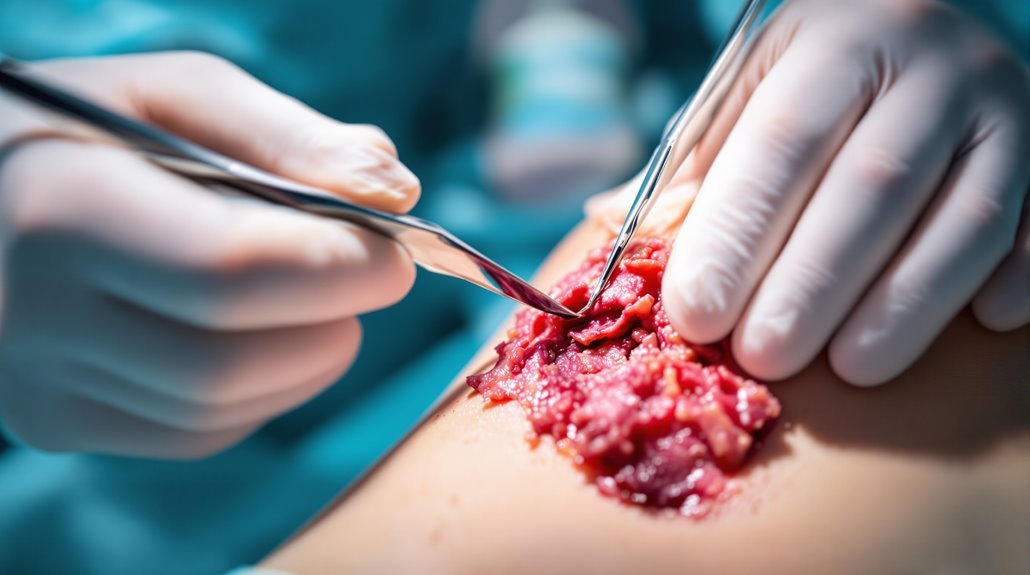
Debridement isn’t just one procedure—it’s a range of techniques healthcare providers use to remove dead, damaged, or infected tissue from wounds and help your body heal.
Understanding the methods of debridement helps you recognize why specialized care matters. Surgical debridement works fastest for extensive wounds, using sterile instruments to eliminate nonviable tissue efficiently.
Surgical debridement uses sterile instruments to rapidly eliminate nonviable tissue—the fastest method for extensive wounds.
Autolytic debridement harnesses your body’s natural enzymes to break down dead tissue gently. Enzymatic debridement applies specialized enzymes directly to accelerate this process.
Mechanical debridement uses physical force through specialized dressings. Even maggot therapy shows promising results for certain cases.
Each method targets your wound’s specific needs, preparing healthy skin for proper wound healing. Your healthcare provider selects the best approach based on wound severity, ensuring effective treatment for recovery.
Surgical Debridement
When your wound requires swift removal of damaged tissue, surgical debridement provides the speed and thorough tissue elimination that other methods can’t match. During this procedure, your surgeon uses a scalpel or specialized scissors to precisely excise infected and necrotic tissue, revealing healthy tissue beneath. They’ll probe the wound depth with a metal instrument to identify any foreign material. The procedure requires anesthesia in a sterile environment.
| Aspect | Details |
|---|---|
| Tools Used | Scalpels or specialized scissors for precision excision |
| Tissue Removed | Infected, hyperkeratotic, and necrotic tissue layers |
| Environment | Sterile surgical setting requiring anesthesia |
Surgical debridement excels at treating chronic wounds that aren’t healing properly. The removal of dead tissue stimulates the wound edges and releases growth factors that reduce inflammation. While it may need repeating to guarantee complete removal, this sharp debridement method gives you the clearest visualization of the wound bed, enabling ideal healing and preventing serious diabetic complications.
Autolytic Debridement

Unlike surgical debridement’s aggressive approach, autolytic debridement harnesses your body’s natural healing processes to gently remove dead tissue.
Your body’s own enzymes work to liquefy necrotic tissue in a moist environment, creating a selective process that preserves healthy tissue while removing only damaged portions.
You’ll benefit from moisture-retentive dressings like hydrocolloids and hydrogels that maintain ideal moisture balance.
This painless method works best for wounds with minimal necrotic tissue and no infection signs. You can receive treatment in outpatient settings or manage it at home, making it accessible.
As you progress through the healing process, regular wound monitoring remains essential.
Watch for complications and guarantee steady progress toward recovery.
This gentle, non-invasive approach makes autolytic debridement an excellent first-line option for serving patients effectively.
Enzymatic Debridement
For more targeted tissue removal, enzymatic debridement applies topical preparations containing specialized enzymes—such as collagenase and papain—directly to your wound bed.
These chemical enzymes work by selectively breaking down and liquefying necrotic tissue without damaging your healthy tissue. Unlike autolytic methods that support your body’s natural healing, enzymatic debridement actively removes dead tissue daily, offering ongoing protection against infection.
You’ll find this approach particularly effective for pressure ulcers, leg ulcers, and burn wounds when adequate blood flow exists. The process helps guide your wound from the inflammatory phase toward the proliferative phase, facilitating cellular migration necessary for epithelialization.
While slower than surgical debridement, enzymatic options spare you the discomfort and anesthesia requirements, making them ideal for outpatient care and promoting healing progress.
Mechanical Debridement
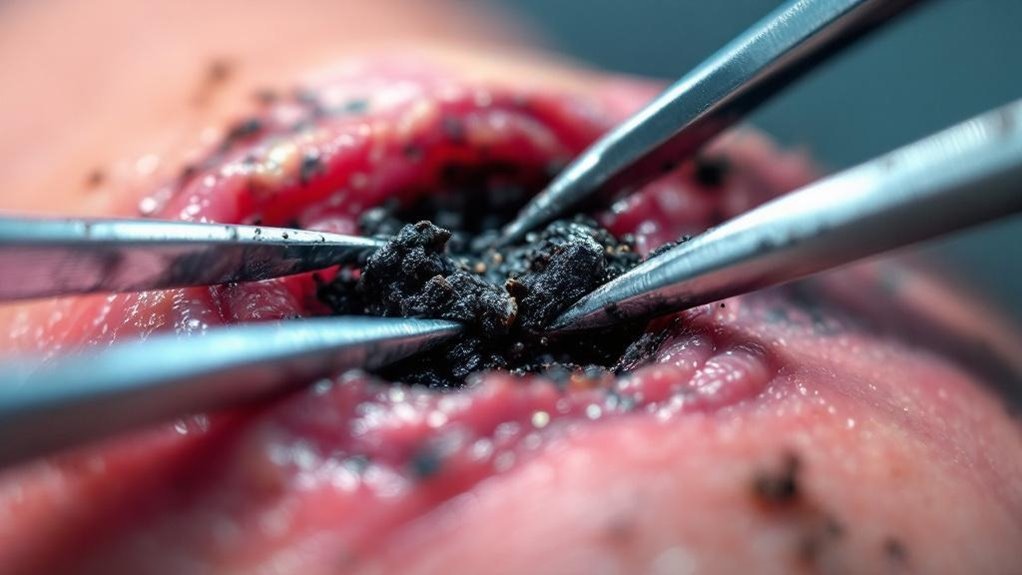
Physical methods form the foundation of mechanical debridement, allowing you to remove dead tissue through direct force application. You’ll find that wound irrigation and therapeutic irrigation are essential techniques you can employ. Hydrotherapy, including pulsatile lavage and whirlpool baths, softens and loosens necrotic tissue quite effectively. You can also use suction with a syringe and catheter for precise cleaning of the wound. Mechanical debridement works best for larger wounds with significant amounts of dead tissue. You’ll need regular sessions to maintain a clean wound bed and promote ideal healing. While this method isn’t selective—potentially removing some healthy tissue—it’s cost-effective and requires minimal special equipment, making it accessible for various care settings. You should consider your patient’s pain tolerance and bleeding risk.
| Technique | Method | Best For |
|---|---|---|
| Wet-to-Dry | Gauze dressings | Initial cleansing |
| Pulsatile Lavage | Pressurized irrigation | Rapid tissue removal |
| Whirlpool | Water immersion | Softening tissue |
Biological Debridement Methods
When evaluating your debridement options, biological debridement—also known as maggot therapy—leverages sterile medical maggots from green bottle flies to selectively remove necrotic tissue while preserving healthy tissue.
These larvae work through multiple mechanisms: they digest dead tissue, ingest harmful bacteria, and release antimicrobial substances that reduce infection risk.
You’ll apply the maggots directly to your wound or place them in a mesh bag, leaving them for 24 to 72 hours before replacement.
This biological debridement method is particularly valuable when dealing with chronic wounds resistant to traditional treatments, antibiotic-resistant infections like MRSA, or when you can’t tolerate surgery.
The process is typically painless and cost-effective, making it an accessible option for wound care that promotes healing while eliminating infection threats.
Main Benefits of Debridement
Debridement removes the tissue that’s actively preventing your wound from healing. When you undergo debridement, you’re giving your healthy tissue a chance to thrive. Dead tissue creates an environment where infection thrives and slows your recovery progress considerably.
By removing nonviable tissue, you’re reducing inflammation and stimulating essential growth factors for effective wound healing and sustained tissue repair. This targeted process prevents serious complications like sepsis and potential amputation risks. You’ll experience faster recovery times as your wound progresses toward proper closure and healthy regeneration. Enhanced blood flow and accelerated cell growth continue to restore damaged areas effectively.
| Benefit | Impact |
|---|---|
| Removes dead tissue | Eliminates barriers |
| Reduces infection | Protects tissue |
| Stimulates growth factors | Accelerates healing |
| Prevents complications | Avoids amputation |
| Improves outcomes | Reduces time |
You’re taking an active role in your complete recovery journey by consciously choosing debridement as your primary treatment path and healing goal.
Preparing for Your Procedure
To guarantee your debridement procedure proceeds safely and effectively, you’ll need to follow several important pre-procedure instructions.
First, inform your doctor about all medications, vitamins, supplements, and herbal remedies you’re currently taking to prevent any potential complications. Stop taking blood thinners if directed. If anesthesia will be used, follow the specific fasting instructions provided.
Inform your doctor about all medications and supplements, stop blood thinners if directed, and follow fasting instructions if anesthesia will be used.
Before your appointment, bathe or shower and carefully avoid applying lotions, perfumes, deodorants, or nail polish to the surgical site.
Don’t shave the area yourself. Remove all jewelry, piercings, and contact lenses. Arrange transportation home if you’ll receive sedation or pain medication, as you won’t be able to drive safely afterward.
Prepare to discuss your complete medical history with your healthcare provider so they can remove the damaged tissue effectively.
Risks and Complications
Like any surgical procedure, debridement carries potential risks and complications you should understand before moving forward. You may experience bleeding, irritation, and damage to healthy tissue surrounding the wound. Allergic reactions to topical agents used during the process can occur.
Pain during and after the procedure is common, so discuss appropriate pain management strategies with your healthcare provider beforehand.
There’s a potential for bacterial infection if proper sterile techniques aren’t carefully followed, making infection prevention especially critical. Additionally, you may experience delayed healing or loss of healthy tissue in some cases.
Despite these risks, the benefits of debridement often outweigh potential complications, as the procedure is essential for promoting wound healing and preventing serious infections. Your doctor will help you weigh these important considerations.
Recovery and Aftercare
Once your procedure is complete, you’re entering a critical healing phase that’ll typically last 6 to 12 weeks, depending on your wound’s severity, size, and location.
Proper wound care forms the essential foundation of your recovery. You’ll keep your wound clean and covered with moist dressings as your care team directs. Monitor healing progress closely and attend all follow-up appointments—these visits guarantee any complications are caught early and your wound closes effectively.
Nutrition plays an important role in your healing journey. Consume adequate protein and nutrients to support tissue regeneration.
Avoid smoking, which greatly impairs blood flow and slows recovery. Practice the specific wound care instructions provided, maintaining dressing changes and keeping the area dry to prevent infection and promote healthy tissue restoration.
Conclusion
You’ll find that debridement’s an essential procedure when you’re dealing with serious or chronic wounds that aren’t healing properly on their own. By removing dead tissue and infected material, you’re actively promoting healing and reducing infection risks. Whether you choose surgical or non-surgical methods, you’re taking a vital step toward recovery. After your procedure, you’ll need to follow proper aftercare and monitor for complications, but you’re setting yourself up for better outcomes and faster healing.