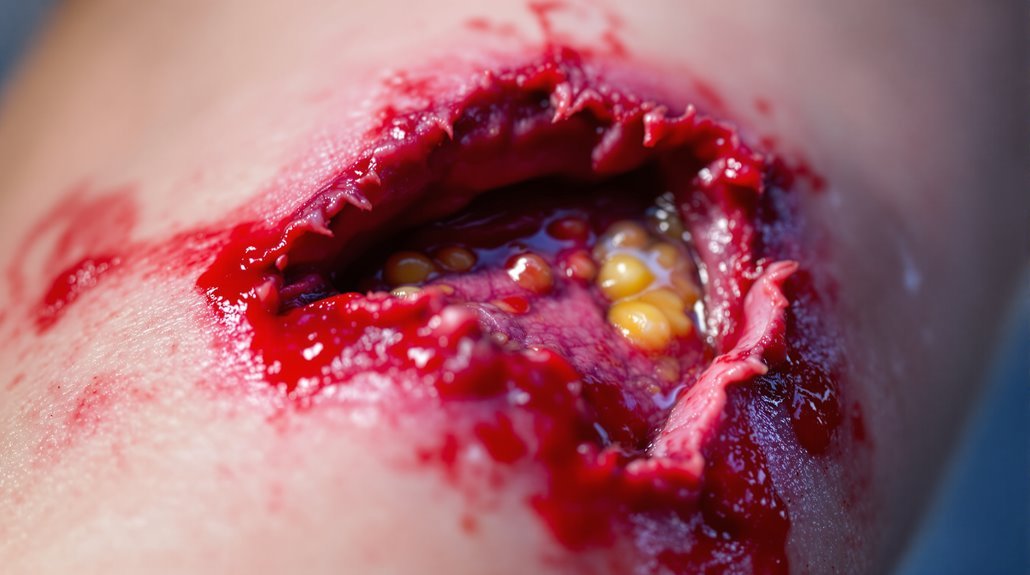
Seek immediate medical attention if your wound bleeds for more than 15 minutes despite firm pressure, exposes internal structures like fat or muscle, or involves animal or human bites. Watch for infection signs including spreading redness, pus, warmth, foul odor, or fever developing within 48-72 hours. You’ll need urgent care if you experience numbness, tingling, or difficulty moving near the wound, or if foreign objects remain embedded. Understanding these critical warning signs and their specific timeframes can help you determine when home care isn’t enough.
Key Takeaways
- Bleeding persists beyond 15 minutes despite firm pressure, indicating potential deep tissue damage requiring emergency care.
- Deep wounds exposing fat, muscle, tendon, or bone need immediate medical attention for proper cleaning and closure.
- Animal or human bites carry high infection risk and may require rabies vaccination or professional wound management.
- Infection signs include spreading redness, warmth, pus, foul odor, fever, or chills developing around the wound.
- Numbness, tingling, loss of sensation, or inability to move limbs suggests nerve or structural damage needing urgent evaluation.
Excessive Bleeding That Won’t Stop With Pressure
When blood continues to flow from a wound for more than 15 minutes despite firm, direct pressure, you’re facing a medical emergency that requires immediate professional intervention.
This excessive bleeding signals potential damage to deeper structures that won’t resolve without medical attention.
Your priority is recognizing when first aid measures aren’t enough. Persistent blood flow indicates severity beyond surface-level injury, risking significant blood loss and shock.
Uncontrolled bleeding beyond 15 minutes demands immediate medical attention—first aid alone cannot address the underlying damage threatening your life.
Don’t remove embedded objects—you’ll worsen the bleeding and complicate treatment.
Transport the injured person to urgent care or emergency services immediately.
While waiting, maintain pressure and keep the wound elevated above heart level when possible.
Your swift action in recognizing uncontrolled bleeding and seeking professional help can prevent life-threatening complications and guarantee proper wound management.
Deep Lacerations or Puncture Wounds
Deep lacerations and puncture wounds expose internal structures—fat, tendons, muscle, or bone—that signal your injury has penetrated beyond the skin’s protective barrier.
These deep lacerations need medical attention for proper irrigation and closure, particularly when they’re gaping or located over joints.
Puncture wounds carry a heightened risk of infection, especially from dirty or rusty objects requiring antibiotics and monitoring.
You’ll need immediate care if the wound resulted from an animal bite, as rabies and cellulitis risks escalate considerably.
Seek urgent treatment when bleeding persists beyond 15 minutes of direct pressure or when the wound exceeds a quarter-inch depth.
Professional evaluation guarantees appropriate closure, minimizes scarring, and prevents serious complications that could compromise your ability to serve others effectively.
Animal or Human Bites
Both animal and human bites require immediate medical attention due to their high bacterial load and infection risk.
You’ll need urgent care if you observe redness, swelling, or pus at the bite site—these indicate developing infection that can progress to cellulitis or systemic complications.
Animal bites carry additional rabies concerns, particularly when vaccination status is unknown.
Post-exposure prophylaxis must be initiated promptly to prevent this fatal disease.
Seek medical attention immediately if the wound is deep or continues bleeding after 15 minutes of direct pressure.
Professional cleaning and closure are essential for proper healing.
Delaying treatment compromises the healing process, leading to severe infections, prolonged recovery, and chronic wound complications.
Your swift action protects those you serve from preventable harm.
Visible Signs of Infection
Recognizing infection early can prevent life-threatening complications like sepsis or tissue necrosis.
You’ll need to monitor for these visible signs of infection: increased redness spreading beyond the wound edges, warmth to the touch, and persistent swelling accompanied by pain.
Wound infection often produces pus or discolored drainage—green, yellow, or brown discharge requires immediate medical attention.
Watch for a foul-smelling odor emanating from the site, which indicates bacterial overgrowth.
A distinctly unpleasant smell from the wound often signals dangerous bacterial colonization requiring prompt medical assessment.
If your patient develops fever or chills alongside wound symptoms, this signals systemic involvement demanding urgent intervention.
Wounds showing no healing progress after several days warrant professional evaluation.
Don’t hesitate to seek medical attention when these indicators appear—early treatment prevents complications and protects those under your care.
Foreign Objects Embedded in the Wound
When foreign objects remain lodged in a wound, they create an immediate pathway for bacteria and prevent proper healing. Glass, metal shards, or dirt embedded beneath the skin aren’t always visible but require professional wound care.
Don’t attempt removal yourself—you’ll risk increased bleeding and tissue damage.
Medical attention becomes critical because healthcare professionals possess specialized tools and expertise to extract foreign objects safely. They’ll assess the wound’s depth, remove embedded materials without compromising surrounding tissues, and implement proper infection prevention protocols.
Even seemingly minor foreign object injuries can develop serious complications if left untreated.
Your prompt action in seeking medical evaluation greatly reduces infection risk and guarantees ideal healing outcomes.
When you’re caring for others with embedded foreign objects, prioritize immediate professional intervention over home remedies.
Wounds That Aren’t Healing Properly
Your body’s wound healing timeline serves as a critical diagnostic indicator—wounds should demonstrate measurable improvement within 48 to 72 hours of injury.
Healthy wounds show visible improvement within 48 to 72 hours—delayed healing signals the need for medical evaluation.
If you’re caring for someone whose cuts and punctures aren’t progressing, recognize that wounds persisting beyond three weeks classify as a chronic wound requiring specialized intervention.
Watch for critical warning signs: persistent bleeding, escalating pain, or discolored drainage. These indicate compromised healing that demands immediate wound care assessment.
Patients with diabetes or immunocompromised conditions need medical attention earlier—don’t wait the full three-day window.
Treatment protocols for non-healing wounds may include debridement, prescription topicals, or advanced therapies like hyperbaric oxygen treatment.
Early intervention prevents complications and accelerates recovery. When healing stalls, prompt medical evaluation isn’t optional—it’s essential for ideal patient outcomes.
Cuts From Rusty or Dirty Objects
Rusty or contaminated objects create puncture wounds that penetrate deep into tissue, bypassing your skin’s protective barriers and depositing Clostridium tetani spores directly into oxygen-poor environments where tetanus thrives. You’ll need immediate medical attention to assess tetanus shot status and prevent complications. Wounds can rapidly become infected when bacteria infiltrate deeper layers.
| Wound Characteristic | Risk Level | Required Action |
|---|---|---|
| Deep puncture | High | Emergency evaluation |
| Visible contamination | High | Thorough debridement |
| Increased redness/swelling | Critical | Urgent care visit |
| Purulent drainage | Critical | Antibiotic therapy |
| No tetanus shot (5+ years) | High | Immediate vaccination |
Proper wound care requires professional cleaning, potential antibiotic administration, and tissue debridement. Don’t delay seeking medical attention—protecting those you serve begins with maintaining your own health and preventing serious complications.
Loss of Sensation or Mobility Near the Wound
Nerve damage transforms a seemingly minor wound into a medical emergency that demands immediate professional assessment.
When you notice loss of sensation, tingling, numbness, or weakness surrounding an injury, you’re observing red flags indicating potential nerve involvement. Impaired mobility near joints suggests tendon or ligament damage requiring prompt diagnosis.
You must recognize that persistent neurological symptoms following trauma can signal crush injuries or fractures—conditions demanding urgent medical evaluation.
Sudden inability to move a limb represents a serious injury potentially requiring surgical intervention. Don’t wait to see if symptoms resolve on their own.
Your prompt action in seeking immediate care protects patients from long-term complications and preserves function.
When sensation disappears or movement becomes impossible, time matters critically for favorable outcomes.
Conclusion
Don’t delay seeking care when you’ve identified these warning signs. Untreated wounds can rapidly progress to serious complications including systemic infection, permanent nerve damage, or tissue death. Contact your healthcare provider immediately if you’re experiencing excessive bleeding, signs of infection, or compromised function. For deep lacerations, embedded objects, or bites, proceed directly to urgent care or your emergency department. Early intervention greatly improves outcomes and prevents long-term complications.