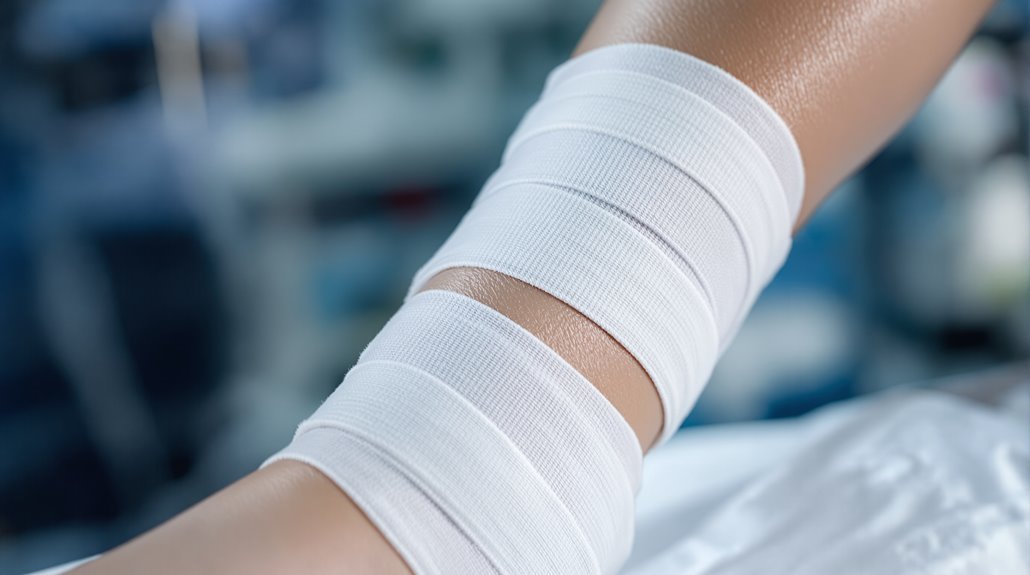
You’ll benefit from compression therapy, which applies graduated external pressure to counteract gravity and restore your venous pump function. It works by reducing distended vein diameter, increasing blood velocity, and improving overall circulation—delivering oxygen and nutrients your leg ulcer needs to heal. The therapy decreases edema, enhances lymphatic drainage, and creates an ideal healing environment. Optimizing your personalized compression approach will greatly impact your recovery, and there’s more to explore about maximizing your treatment.
Key Takeaways
- Compression therapy reduces distended vein diameter, increasing blood velocity and oxygen delivery for effective venous ulcer healing.
- Compression significantly reduces ulcer recurrence: 210 per 1000 with compression versus 457 without, demonstrating substantial preventive effectiveness.
- Multi-layer bandaging systems and compression hosiery deliver graduated pressure (measured in mmHg) tailored to individual ulcer severity.
- Absolute contraindications include severe peripheral arterial disease, uncontrolled heart failure, and untreated infections; screening via ankle-brachial index testing is essential.
- Long-term adherence to compression therapy prevents recurrence; balancing therapeutic pressure with wearability improves patient compliance and health outcomes.
Understanding Compression Therapy
Compression therapy harnesses controlled external pressure applied to the lower leg to counteract gravitational forces and restore proper venous function.
By harnessing controlled external pressure, compression therapy counteracts gravity to restore proper venous function.
You apply graduated compression through bandages or specialized hosiery that progressively reduces pressure from ankle to knee, enhancing blood velocity toward the heart.
This mechanism addresses the underlying pathophysiology of venous ulcers by reducing distended vein diameter and improving lymphatic drainage.
You’ll find that effective compression therapy reduces edema, facilitates tissue remodeling, and creates an ideal healing environment by delivering essential oxygen and nutrients to ulcerated tissue.
The therapy works systematically—compressing the calf muscle, which functions as a venous pump, proves particularly critical.
How Compression Therapy Works
The therapeutic benefits of compression stem from a straightforward physiological principle: externally applied pressure generates a gradient that restores normal venous hemodynamics.
When you apply compression bandages, you’re reducing the diameter of distended veins, which increases blood velocity and enhances venous return toward your heart. This improved circulation delivers oxygen and nutrients essential for healing venous ulcers effectively.
By carefully managing venous insufficiency through controlled pressure, you’re minimizing fluid buildup and reducing peripheral edema formation. Multi-layer bandaging systems allow you to adjust pressure levels based on your condition’s severity.
You’ll experience reduced swelling and improved lower limb wound healing. Graduated compression hosiery provides consistent therapeutic pressure throughout the day, supporting your body’s natural healing mechanisms.
This straightforward mechanical intervention markedly accelerates your recovery process.
Types of Compression Systems
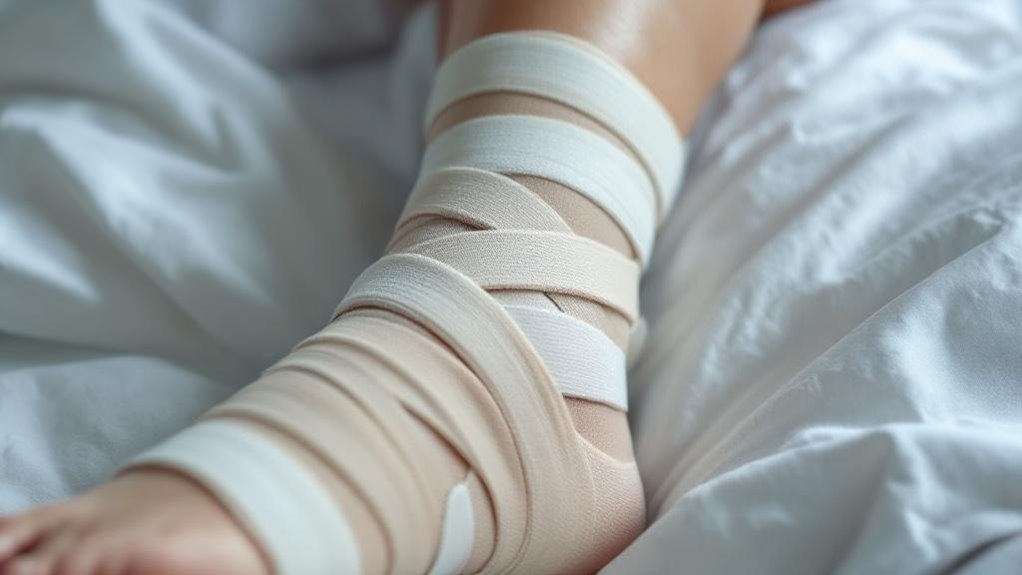
Several compression systems are available to address your therapeutic needs, each engineered to restore venous function through distinct mechanical approaches.
You’ll utilize multi-layer bandaging systems in 3–4 layer formats that provide effective graduated pressure to promote venous return and facilitate ulcer healing processes.
Compression hosiery, classified by pressure levels at the ankle, offers tailored options ranging from light to extra-high performance for varying individual patient needs.
Compression hosiery offers pressure-customized solutions, ranging from light to extra-high performance, tailored for individual venous insufficiency management needs.
These precise levels of compression—typically measured in millimeters of mercury (mmHg)—allow you to tailor evidence-based interventions for individual patients managing chronic venous insufficiency and progressive vascular disease.
Your specific treatment selection depends directly on ulcer severity and swelling extent.
You’ll apply bandages during active wound phases while reserving compression hosiery for ongoing maintenance and prevention post-healing.
Compression Bandaging Techniques
Multi-layer bandaging systems represent the primary therapeutic approach for active venous leg ulcers, delivering graduated compression through typically 3–4 elasticated layers.
You’ll apply these layers systematically: a non-adherent wound contact layer, padding protecting bony prominences, light compression layers, and a high-compression outer layer.
You’ll stretch bandages to approximately 50% of maximum elasticity using spiral or figure-of-eight techniques, ensuring the highest pressure concentrates at the ankle.
You’ll wrap from toes to just below the knee, maintaining graduated pressure that progressively decreases toward the calf. This graduated approach enhances blood flow toward the heart, actively reducing venous pooling and edema.
You’ll monitor application carefully—improper technique compromises effectiveness and risks patient harm.
You’ll change bandages regularly, typically 1–3 times weekly, maintaining consistent therapeutic pressure throughout healing.
Compression Hosiery and Stockings
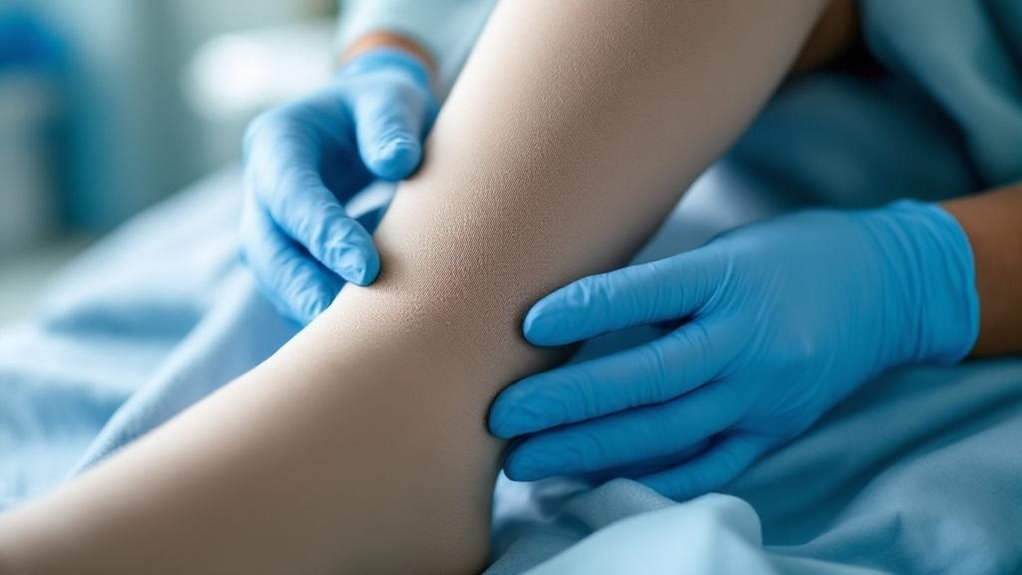
Compression stockings shift you from acute bandage management to long-term prevention, delivering graduated pressure that progressively decreases from ankle toward calf.
These medical devices come in standardized compression classes—from light (18-21 mmHg) to very strong (49+ mmHg)—allowing you to match therapeutic intensity to your patient’s clinical needs.
Class 3 compression demonstrates superior effectiveness, considerably lowering recurrence rates of venous ulcers compared to lower classes.
Class 3 compression demonstrates superior effectiveness, considerably reducing venous ulcer recurrence compared to lower therapeutic classes.
You’ll apply these stockings for extended periods post-healing, maintaining optimized circulation and preventing new ulcer formation.
Proper fitting remains absolutely critical; misfitting compromises efficacy and creates complications.
Partner closely with your patients during fitting to guarantee comfort and compliance.
Professional evaluation determines the appropriate compression class, assuring you’re preventing recurrence through evidence-based, individualized intervention rather than generic approaches.
Contraindications and Safety Considerations
While you work to optimize healing with compression therapy, you must first identify and rule out absolute contraindications that can severely compromise patient safety.
You’ll screen patients for severe peripheral arterial occlusive disease with ankle-brachial pressure index below 0.6, uncompensated heart failure, and untreated active infections before applying compression.
You should also identify advanced diabetic neuropathy and sensory loss risks, which demand careful consideration.
Proper fitting of compression garments is essential for both effectiveness and patient safety—misfitting can cause discomfort or tissue damage.
You must monitor patients closely for warning signs including numbness, unusual pain, or excessive swelling after application.
When you encounter contraindications, you’ll consult colleagues to determine whether modified compression approaches might benefit the patient while maintaining appropriate safety standards.
Maximizing Patient Adherence
Once you’ve confirmed that compression therapy is appropriate for your patient, you’ll recognize that treatment success depends heavily on ongoing adherence to the prescribed regimen.
You can greatly improve patient outcomes by tailoring compression methods to individual needs and comfort levels. Providing thorough education about therapy benefits and proper application enhances patient understanding and encourages compliance.
Regular follow-ups allow you to address specific barriers your patients face and systematically monitor concerns like discomfort or skin reactions—issues that commonly undermine commitment to treatment.
By providing consistent support and regularly tracking therapeutic progress, you’ll help patients maintain their compression regimen long-term.
Given that approximately 1% of adults may experience leg ulcers, robust patient adherence prevents ulcer recurrence and considerably improves overall quality of life outcomes.
Preventing Ulcer Recurrence
After your patient’s venous ulcer heals, maintaining consistent compression therapy becomes critical to preventing recurrent ulceration.
European class 3 compression stockings greatly reduce recurrence risk—only 210 of every 1000 patients experience ulcer recurrence, compared with 457 without compression.
Stronger devices with pressure ≥30 mm Hg don’t just reduce recurrence risk effectively; they remarkably extend the interval between ulcer episodes.
You’ll want to make sure your patients apply correct pressure levels continuously and fully understand why long-term adherence matters for their health outcomes.
However, higher compression classes can compromise long-term compliance rates, so you’ll need to balance therapeutic effectiveness with realistic wearability.
Providing thorough interdisciplinary education combined with consistent follow-up communication strengthens your patients’ commitment to lifelong compression use, ultimately safeguarding against costly recurrent ulceration.
Conclusion
You’ll find compression therapy is the gold standard treatment for venous ulcers—it’s the most evidence-supported clinical intervention available today. When you apply appropriate compression, ideally greater than 20 mmHg, you’ll achieve faster ulcer healing and markedly reduced pain compared to no compression. You must maintain compression long-term to prevent ulcer recurrence, using graduated compression from ankle to calf. Your clinical success depends on patient adherence, as consistent therapy considerably reduces recurrence rates.