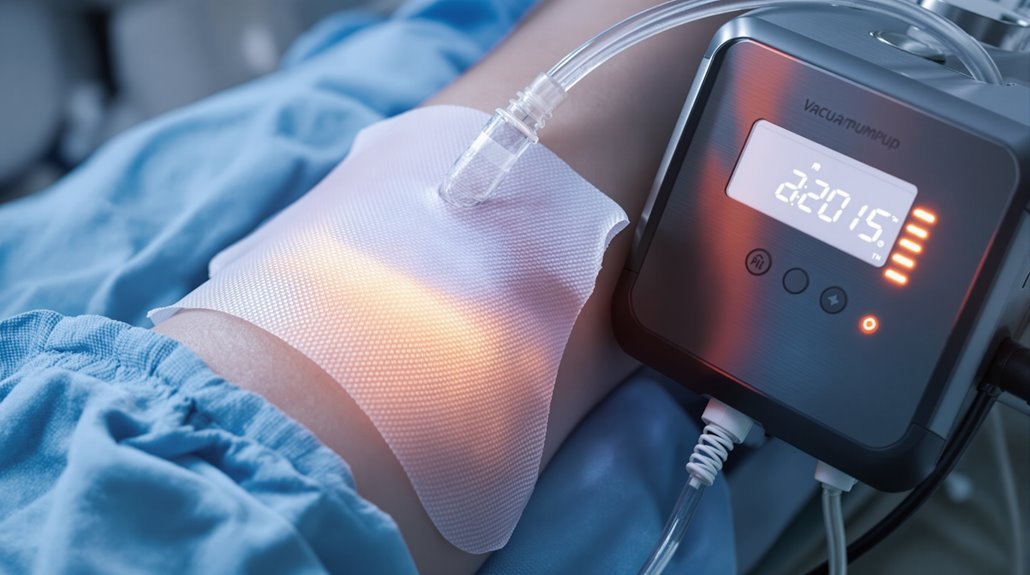
When you apply negative pressure wound therapy, you’re using a vacuum-assisted closure system creating subatmospheric pressure on your wound. This sealed environment removes excess fluid and infectious materials while stimulating cellular growth and angiogenesis. The foam dressing compresses to pull your wound edges together, reducing surface area and promoting faster granulation tissue formation. You’ll experience dressing changes every 48-72 hours, maintaining a moist healing environment. Learn how this therapy delivers clinical benefits for complex wounds.
Key Takeaways
- Negative Pressure Wound Therapy applies subatmospheric pressure to wounds, removing excess fluid and infectious material while promoting granulation tissue formation and faster healing.
- NPWT uses a sealed foam dressing connected to a vacuum pump that maintains approximately -125 mmHg pressure to compress wounds and stimulate cellular activity.
- Benefits include accelerated healing rates, reduced infection risk, fewer dressing changes, improved patient comfort, and higher graft-take rates with skin grafting procedures.
- NPWT effectively treats chronic wounds, pressure ulcers, acute wounds, surgical wounds, and complex traumatic injuries resistant to traditional wound management approaches.
- Potential complications include bleeding, pain during dressing changes, foam adhesion to tissue, skin irritation, and infection concerns requiring continuous monitoring and assessment.
What Is Negative Pressure Wound Therapy?
Negative Pressure Wound Therapy (NPWT), commonly called vacuum-assisted closure or VAC therapy, is a medical treatment promoting wound healing by applying subatmospheric pressure to the wound surface.
You’ll place a foam dressing into the wound, cover it with adhesive film, and connect a vacuum pump that creates negative pressure. This environment removes excess fluid and infectious materials while stimulating granulation tissue formation.
NPWT’s effectiveness makes it ideal for treating pressure ulcers, chronic wounds, and complex injuries requiring intensive wound care.
NPWT effectively treats pressure ulcers, chronic wounds, and complex injuries requiring intensive wound care.
You’ll change the dressing every 48 to 72 hours in an outpatient setting, allowing patients to continue their lives while healing progresses.
This portable approach considerably accelerates recovery and reduces infection risk, making Negative Pressure Wound Therapy an essential tool in modern wound management.
How Negative Pressure Wound Therapy Works
When you establish negative pressure at approximately -125 mmHg on the wound surface, the sealed foam dressing compresses to roughly 80% of its original size. This macrodeformation directly pulls the wound edges together while reducing the wound’s surface area.
Simultaneously, suction through the foam’s pores creates microscopic stress that stimulates cellular activity and promotes robust angiogenesis. The NPWT systems you’ll use remove excess inflammatory exudate, maintaining a moist wound environment while reducing edema and tissue swelling.
The airtight adhesive film seals the foam dressing, enabling consistent suction delivery. Microdeformation—the microscopic tissue rippling—promotes granulation tissue formation and accelerates wound healing.
You’ll perform dressing changes every 48 to 72 hours, carefully monitoring progress while maintaining the negative pressure essential for complete tissue regeneration.
Benefits of NPWT
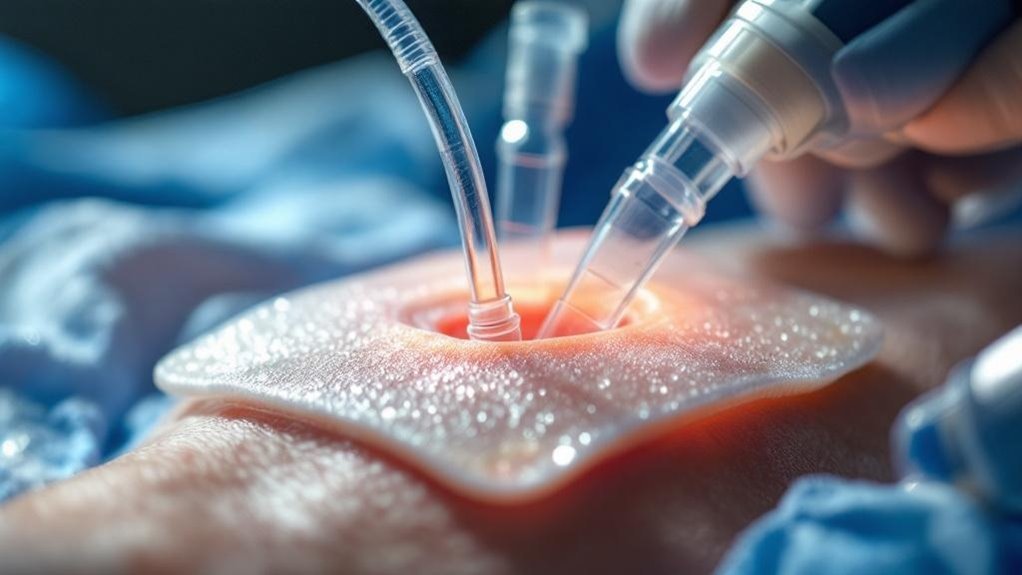
Because the mechanical effects of negative pressure operate at the cellular and tissue level, NPWT delivers substantial clinical benefits across multiple wound categories and patient populations.
You’ll accelerate healing rates—research demonstrates that pressure wound therapy promotes faster granulation tissue formation and re-epithelialization compared to traditional wound dressing methods.
The sealed environment through drainage tubing removes infectious material and excess fluid while reducing edema, creating ideal conditions for tissue regeneration.
For chronic and acute wounds, you’ll reduce dressing changes to 48-72 hours, enhancing patient comfort and decreasing visits.
When used with skin graft procedures, you’ll achieve higher graft-take rates.
Potential Risks and Side Effects
While NPWT powerfully accelerates wound healing, the mechanical forces driving its benefits don’t come without risks you’ll need to recognize and manage.
| Complication | Cause | Management |
|---|---|---|
| Bleeding | Suction pressure on fragile blood vessels | Monitor closely; adjust pressure settings |
| Pain | Dressing changes and wound site pressure | Implement appropriate pain management strategies |
| Foam Adhesion | Dressing material sticking to newly formed tissue | Careful removal; protect tissue bed |
You’ll encounter infection concerns, as NPWT may not eliminate all bacteria present in wounds. Skin irritation from adhesive materials requires vigilant monitoring during application. Some patients experience allergic reactions. Proper monitoring during dressing changes helps you prevent serious complications and guarantee peak healing outcomes for those you serve. Recognizing these risks empowers you to deliver safer, effective wound care.
Candidacy for NPWT Treatment

Determining NPWT candidacy requires you to weigh its healing potential against absolute contraindications and individualized risk factors.
You’ll find NPWT particularly beneficial for chronic wounds—such as stage III and IV pressure ulcers and diabetic lower-extremity ulcers—where it enhances granulation tissue formation. Recent traumatic or surgical wounds with high-volume drainage also benefit from this treatment.
However, you must assess for critical contraindications including untreated osteomyelitis, malignancy, and necrotic tissue before initiating treatment.
Your assessment should incorporate a thorough wound care program addressing underlying conditions like diabetes and nutritional status.
You’ll need to implement continuous monitoring throughout treatment, with formal reassessment every 14 days.
This monitoring determines treatment effectiveness and necessity for continuation, ensuring you’re providing ideal care tailored to each patient’s healing trajectory.
What to Expect During Treatment
During NPWT treatment, your wound undergoes a series of coordinated interventions designed to optimize healing. Your healthcare provider carefully secures layers of foam dressing around your wound’s contours, then seals it securely with adhesive film to create a complete airtight environment. The vacuum pump connects to this sealed dressing, delivering controlled negative pressure that systematically draws exudate and infectious materials from your wound bed.
| Component | Function |
|---|---|
| Foam dressing | Wound coverage |
| Adhesive film | Airtight seal |
| Vacuum pump | Negative pressure delivery |
| Collection canister | Exudate collection |
| Monitoring system | Treatment assessment |
Dressing changes occur every 48 to 72 hours, depending on your wound condition and overall drainage volume. Throughout your active treatment course, your care team maintains continuous monitoring of the dressing’s seal, pump settings, and wound output. Pain management strategies are actively employed during dressing changes to enhance your comfort, ensuring you’re engaged in your healing journey and overall success.
When to Contact Your Healthcare Provider
How can you identify when your symptoms warrant immediate healthcare contact?
You’ll need to reach out to your healthcare provider immediately if you experience excessive bleeding from the wound, as this signals a serious complication requiring immediate medical intervention.
Monitor for fever during your NPWT treatment—it often indicates infection necessitating prompt medical evaluation and proper assessment.
Monitor for fever during NPWT treatment—it often indicates infection requiring prompt medical evaluation.
Check that your wound dressing maintains a proper seal; a loose seal compromises therapy effectiveness and overall healing progress considerably.
You should report any unusual device sounds, low battery alerts, or blockages in the drainage tube, as these indicate critical malfunctions affecting your NPWT performance and safety.
If your device stops unexpectedly, contact your healthcare provider to prevent delays in wound healing and address potential complications promptly.
Conclusion
You’ll benefit from NPWT’s multi-faceted approach to wound healing. By applying negative pressure through a sealed dressing system, you’re drawing out excess fluid while simultaneously promoting granulation tissue formation and improving blood circulation. You’ll experience reduced infection risk and accelerated healing across various wound types—from diabetic foot ulcers to surgical incisions. You’ll need regular dressing changes every 2-5 days, but you’re gaining an effective, evidence-based therapy that’s transformed modern wound care since the 1990s.