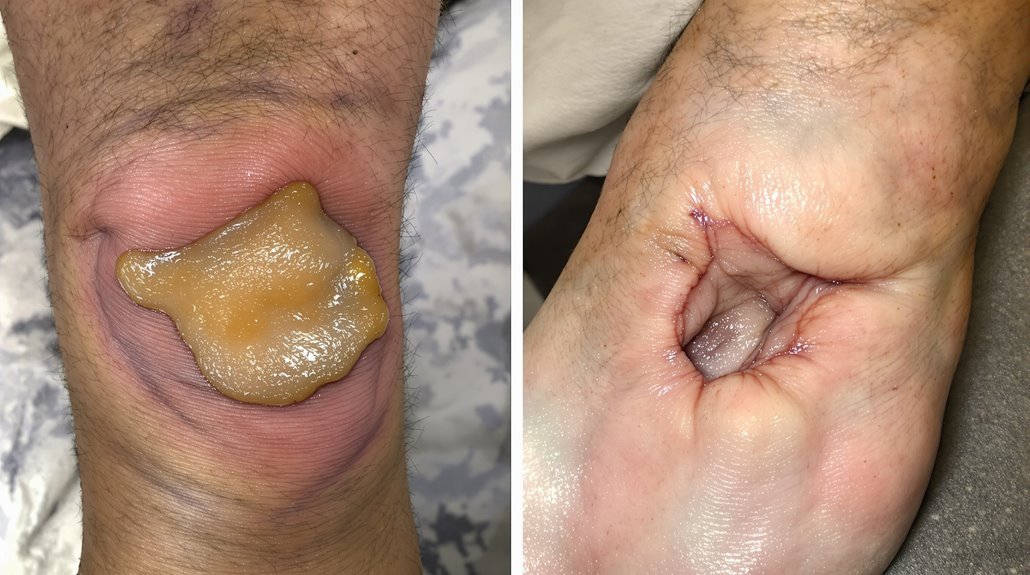
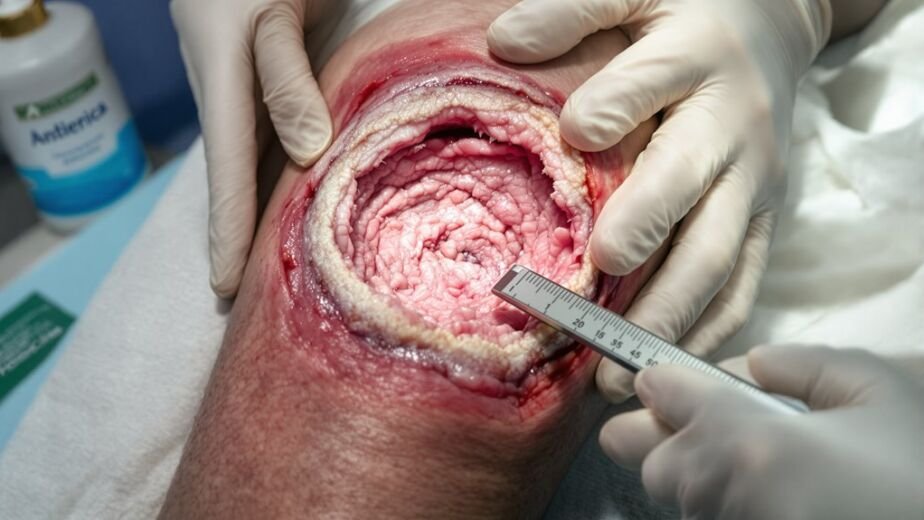
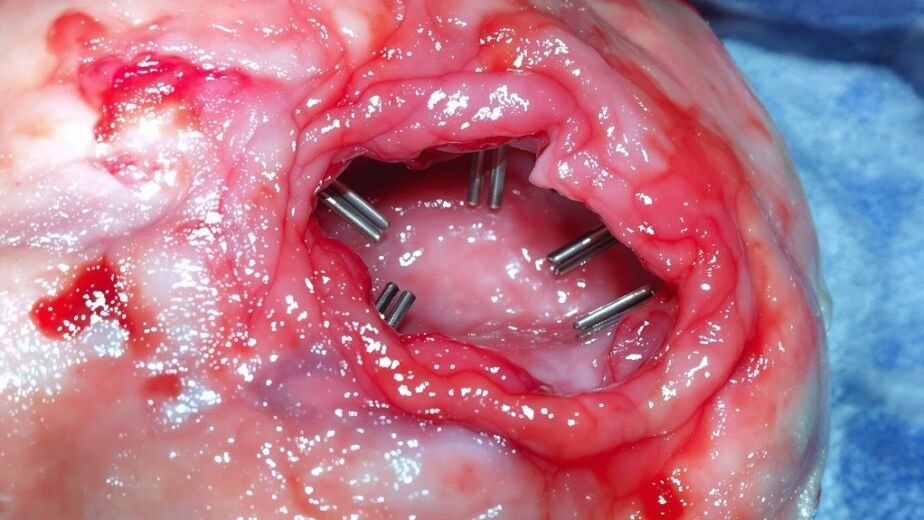
You’re fighting two opposite circulatory problems—arterial versus venous ulcers. Arterial ulcers stem from blocked arteries, creating deep, painful wounds on your toes or heels that worsen with elevation. Venous ulcers result from valve failure, causing larger, shallower sores above your ankle that improve with elevation. Skin appearance differs: arterial shows cool, shiny skin while venous displays swelling. Treatment diverges—arterial needs blood flow restoration while venous needs compression. Which you’re fighting shapes your recovery.
Key Takeaways
- Arterial ulcers appear on toes, heels, or outer ankle; venous ulcers develop above the inner ankle.
- Arterial ulcers are small, deep, and round with well-defined borders; venous ulcers are larger, shallow, and have irregular borders.
- Arterial ulcers cause severe pain worsening with leg elevation; venous ulcers produce dull aches that improve with elevation.
- Arterial ulcer skin appears shiny and cool; venous ulcer skin shows swelling and discoloration.
- Arterial ulcers require vascular surgery to restore blood flow; venous ulcers respond to compression therapy and elevation.
What Are Arterial and Venous Ulcers?
Arterial and venous ulcers represent two fundamentally distinct vascular wounds that develop from different circulatory failures and underlying causes.
Arterial ulcers form when blocked arteries restrict blood flow to your extremities, creating deep wounds with well-defined edges on your toes, heels, or outer ankle.
Venous ulcers result from valve failure in your veins, causing blood pooling and irregular-bordered wounds just above your ankle with warm, discolored, swollen skin.
You’ll experience severe pain with arterial ulcers, especially when elevating your leg, whereas venous ulcers present a dull ache that improves with elevation.
Characteristics differ: arterial ulcers appear shiny and cool, while venous ulcers show swelling and discoloration.
Treatment diverges—arterial ulcers require surgery to restore circulation, venous ulcers use compression therapy.
Causes of Arterial and Venous Ulcers
Understanding what causes these ulcers explains why they require such different treatment strategies.
Arterial ulcers develop when you’re dealing with poor circulation—specifically, ischemia resulting from narrowed or blocked arteries. This inadequate blood flow typically stems from peripheral artery disease, diabetes, high cholesterol, smoking, and advanced age.
> Arterial ulcers develop from poor circulation—ischemia caused by narrowed or blocked arteries, often stemming from diabetes, high cholesterol, smoking, and advanced age.
Venous ulcers, conversely, arise from venous insufficiency where damaged veins cause blood pooling and increased venous pressure. Risk factors include varicose veins, obesity, previous blood clots, prolonged immobility, and older age.
Both conditions can initiate from minor injuries, but their underlying pathophysiology differs fundamentally. You’ll find approximately 70-90% of lower extremity ulcers are venous, while only 5-10% stem from arterial disease.
Understanding these distinct causes helps guide your accurate diagnosis and appropriate clinical intervention for your patients.
Key Differences in Symptoms and Characteristics
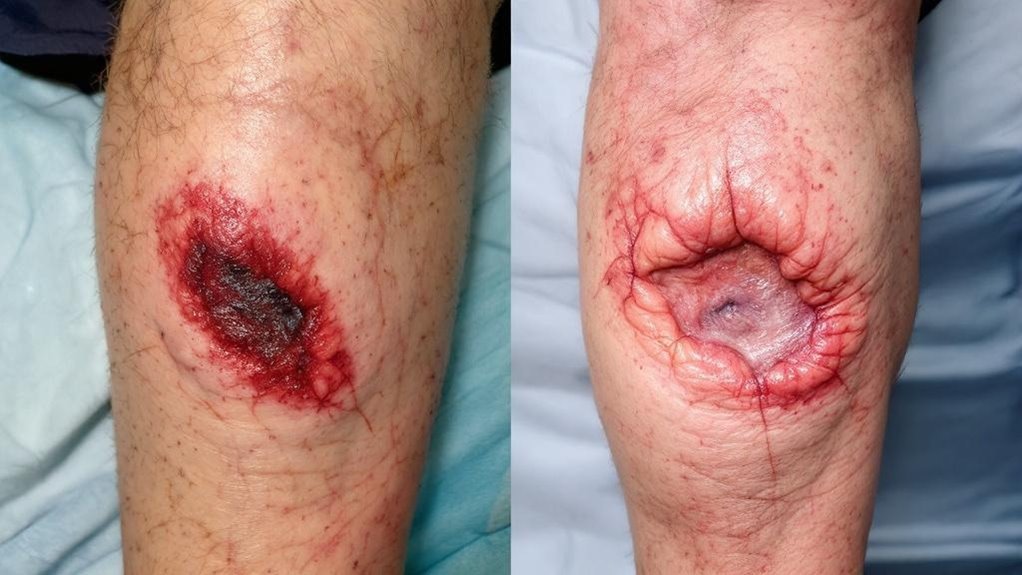
Since these ulcers develop from opposite vascular pathologies, they present with distinctly different clinical characteristics that enable straightforward differentiation.
You’ll observe arterial ulcers are small, deep, round with well-defined borders, while venous ulcers appear larger, shallow, and irregular.
Pain levels differ dramatically—arterial ulcers cause severe pain worsening with elevation, whereas venous ulcers produce dull aches improving with height.
The skin surrounding arterial ulcers appears shiny, hairless, cool, contrasting with warm, discolored, swollen skin around venous ulcers.
Drainage patterns distinguish these wounds: arterial ulcers have minimal or pale bluish drainage, while venous ulcers exhibit moderate to heavy drainage with ruddy appearance.
Location matters—arterial ulcers develop on toes, heels, ankles in your lower extremities, whereas venous ulcers form above medial malleolus affecting blood flow.
Pain Levels and Location: How They Compare
Though both ulcers damage the lower extremities, their pain characteristics and anatomical distributions differ fundamentally: you’ll experience severe, sharp pain with arterial ulcers that worsens when you elevate your leg, whereas venous ulcers cause a dull ache that improves with elevation.
Arterial ulcers develop on the outer ankle, toes, heels, or pressure points, presenting with “punched out” ulcer edges and cool surrounding skin. This intense, resting discomfort reflects severely compromised blood flow to tissues.
Venous ulcers locate just above the medial malleolus on your inner lower leg, featuring irregular borders and warm, swollen surrounding skin. The discomfort you experience intensifies toward day’s end due to chronic venous insufficiency.
Understanding these pain levels and location distinctions helps you identify which type requires intervention and treatment.
Treatment Approaches for Each Type
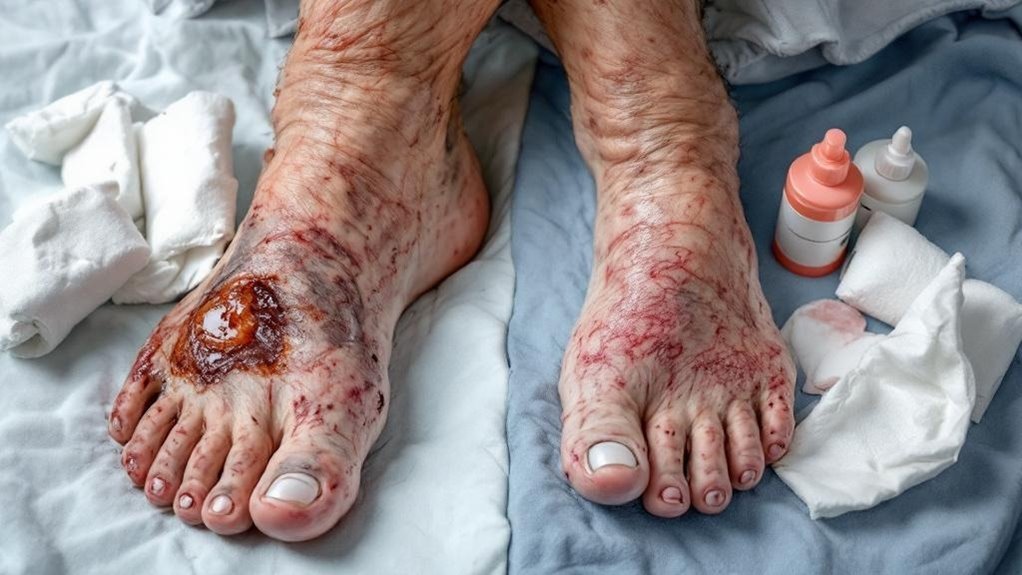
Because the underlying mechanisms driving arterial and venous ulcers differ, your treatment strategies must also diverge markedly. For arterial ulcers stemming from poor blood circulation, you’ll focus on restoring blood flow through surgical interventions like angioplasty or bypass surgery to address the underlying vascular compromise effectively. For treatment for venous ulcers, you’ll prioritize compression therapy combined with leg elevation and thorough wound care protocols specifically designed to heal the ulcer and prevent recurrent complications. Your approach hinges on understanding the distinct underlying cause—inadequate arterial perfusion versus chronic venous insufficiency affecting tissue oxygenation and perfusion.
| Aspect | Arterial Ulcers | Venous Ulcers |
|---|---|---|
| Primary Goal | Restore blood circulation | Reduce edema and swelling |
| Main Treatment | Vascular surgery/angioplasty | Compression therapy |
| Wound Care | Antibiotics and protection | Dressings and elevation |
| Healing Timeline | Slower, often prolonged | Typically 3-4 months |
| Adjunctive Therapy | Pain management protocols | Topical treatments/dressings |
You’ll recognize both types require antibiotics to prevent infection, though they won’t independently heal the ulcer. By tailoring interventions to each ulcer’s unique pathophysiology, you’ll markedly improve patient outcomes and healing success.
Prevention and Risk Factor Management
Prevention greatly outpaces treatment in effectiveness, particularly when you understand your risk profile and implement targeted interventions before ulceration occurs.
You’ll notably reduce your risk by maintaining a healthy weight and engaging in regular physical activity, both enhancing circulation and blood flow to your extremities. Managing chronic conditions—including high blood pressure, high cholesterol, and diabetes—directly decreases your likelihood of developing arterial ulcers.
For venous ulcer prevention, compression therapy and leg elevation are essential strategies that minimize swelling and promote venous return. You should inspect your feet regularly, treating minor injuries promptly, and wear appropriate footwear while avoiding prolonged standing or sitting.
These targeted risk factor interventions create thorough prevention strategies protecting you from both ulcer types while supporting your long-term wellness goals.
Conclusion
You’ll find that distinguishing between arterial and venous ulcers is absolutely essential for successful treatment outcomes. Arterial ulcers demand revascularization procedures to restore blood flow, while venous ulcers require compression therapy to improve venous return and reduce hypertension. By recognizing their distinct presentations—arterial ulcers’ severe, localized pain and deep “punched-out” appearance versus venous ulcers’ shallow, irregularly bordered wounds with moderate drainage—you’ll guarantee timely, evidence-based interventions that prevent serious complications and promote ideal healing.